For medical students and professionals engaging in continuing education, rapid technological advancements have dramatically impacted the learning experience.
Augmented reality (AR) provides medical students with simulated, hands-on experiences regarding the exploration of the human body and how it functions. While it’s still common practice to autopsy real cadavers, AR enables learners to practice without performing an actual autopsy.
Let’s take a look at simulated anatomical models and the presence of AR in medical education, as well as instances when a real-life cadaver is still required for an autopsy for educational purposes.
1) The Cadaver as an Essential Part of Learning
Traditionally, medical students learn about the human body and surgical methods using cadavers, which are deceased human bodies. Most medical schools mandate cadaver dissection as a necessary part of understanding and identifying human anatomy.
Using cadavers, however, can be costly and time-consuming for the modern medical student, who could just as easily learn on virtual models. VR and AR have been lauded as inexpensive ways to improve access to medical education.
While virtual models prove useful, allowing students to choose the angle at which they view internal structures, critics argue that virtual cadavers currently lack adequate capabilities in some areas, such as haptic (touch-related) understanding of various anatomical features.
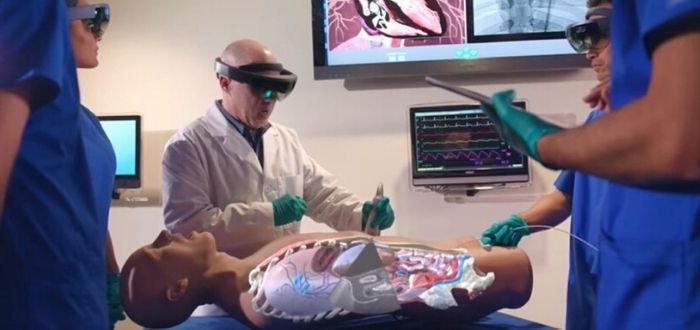
2) Immersive Learning
Immersive experiences enable students to learn by doing. They can confront emergency-level situations in an immersive learning environment.
With Immersive Learning, students can train themselves to deal with panic, mistakes, and other life-changing difficulties that can occur in an operating room or during an emergency.
For these reasons, the virtual reality industry in healthcare may reach $5.1 billion by 2025. This is life-saving technology, not just in diagnostic arenas, but in education and even virtual office space development.
Also Read: How Machine Learning and AI are Changing Healthcare
3) The Virtual Patient: An Educational Staple and a Future Reality
Imagine putting on a virtual reality (VR) headset. Instead of conducting telemedicine over a video interface, you’re sitting with a patient located across the world.
They may speak Mandarin, but it’s auto-translated to English. While they’re physically located in China, a virtual representation stands before you. You can observe, touch, and even X-ray the patient.
Instead of working with a real patient, students could train using a simulated copy of an individual’s experiences.
Virtual patients are already helping medical students in supervised medical practice. In future, virtual patients could become standard practice in medical education.

4) Integrated Technology: Traditional Learning Methods Plus Tech
In some cases, medical students learn using integrated technology. This includes traditional learning methods, such as practising on an anatomical model, with a technological element added. In this example, the anatomical model would be equipped with nodes and sensory input. In this way, educators rely on time-tested methods with a technological edge.
These integrated methods also work with task-trainer platforms and role-play scenarios with technical elements (such as expecting the medical student to assess a role player and input information into a simulated medical database).
Studies show that integrated technological learning for nurses has become particularly valuable in the paediatrics and obstetrics fields. This technology directly benefits patients, and medical professionals need training on how to apply it.
Also Read: How Blockchain is Shaping the Healthcare Industry
5) Augmented Reality Beyond Medical Education
Technological advancements in the medical field aren’t just limited to medical education. Augmented reality has been used to help patients suffering from phantom limb pain, which occurs when someone loses a limb.
When an amputee patient’s muscles send out electrical signals, augmented reality serves as a receptor, resulting in minimal to no pain for a patient who previously experienced pain at the amputation site.
Final Thoughts
Augmented and virtual realities are here to stay in the world of medical education. In future, almost all doctor-patient relationships will be virtual, with fewer in-person visits mandated.
Combined with 3D printing technology, mailed prescription services, and other technology, advancements healthcare education are destined to expand rapidly.
